The Chaos Has a Pattern: What's Really Happening to Your Hormones in Perimenopause
Publication 11
The Reality of Hormonal Transition
If your cycle has started doing things it's never done before — skipping months, arriving early, hitting you harder emotionally — there's a good chance perimenopause has already begun. For most women, this transition starts years before periods actually stop, and the hormonal shifts driving it are more complex than most of us were ever told. This breakdown is based on a 2018 review published in Obstetrics and Gynecology Clinics of North America, which synthesized decades of longitudinal research on how hormones change during the menopausal transition and how those changes connect to the symptoms women actually experience.
The Big Picture:
A Shift, Not a Shutdown
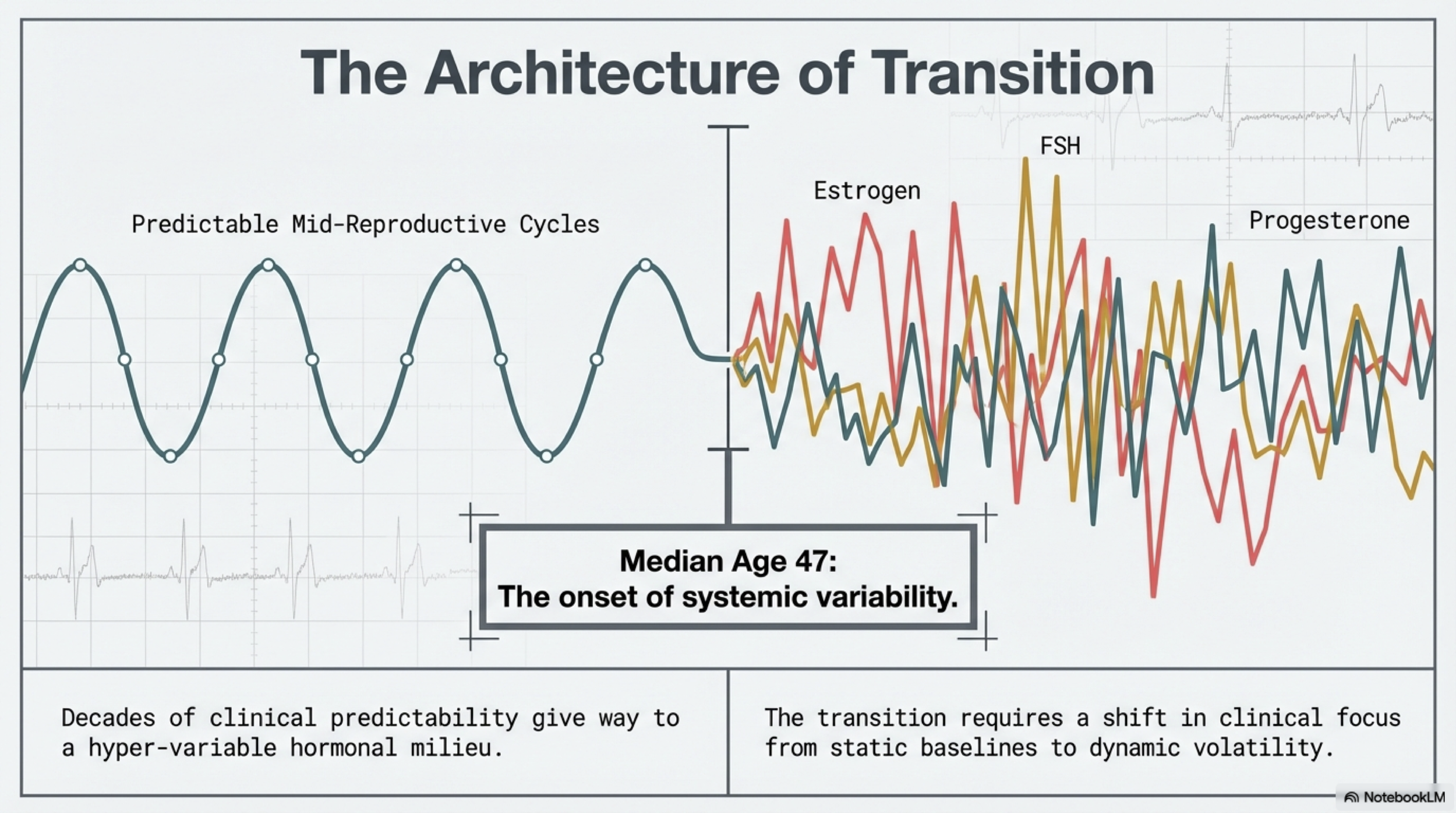
Most of us were taught that menopause is when your periods stop. That's technically true, but it misses almost everything important.
The transition begins years before your final period, when your body's hormonal command center — the hypothalamic-pituitary-ovarian (HPO) axis — shifts from decades of relative predictability into a phase of significant variability. The official marker researchers use is the Final Menstrual Period (FMP), but the hormonal turbulence typically starts long before any cycle change you'd notice.
Your chronological age is also a surprisingly poor predictor of where you are in this process. While the median age for the transition to begin is around 47, the more telling indicators are the hormonal shifts happening beneath the surface — often before your cycles show any outward disruption.
The Research Behind This: Why Study Design Matters
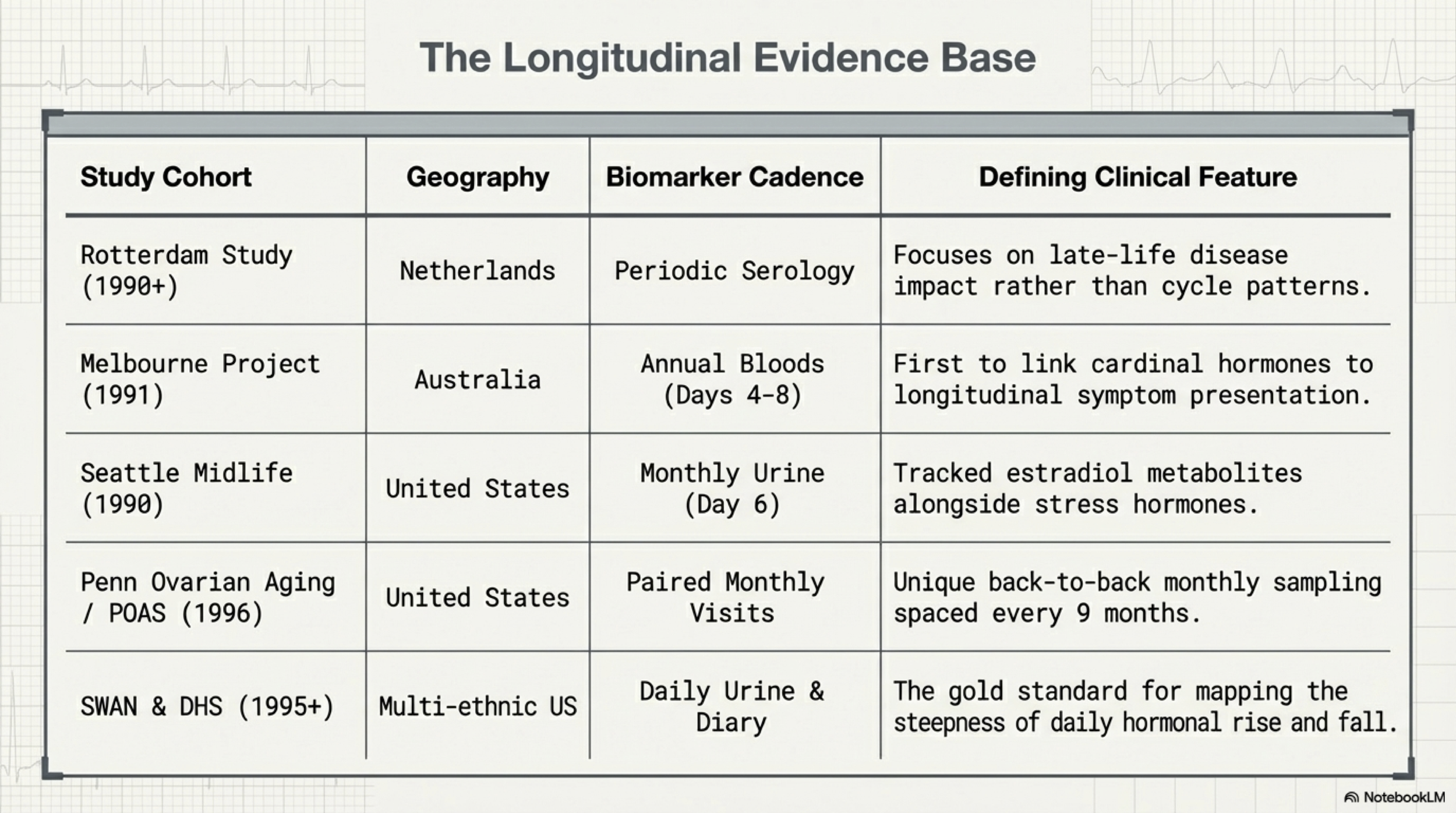
The quality of what we understand about perimenopause depends entirely on how it was studied. A cross-sectional study gives you a single snapshot — useful for spotting patterns, but unable to show how any one person changes over time. Because sex hormones fluctuate far more consistently within an individual than across a population, the most valuable research is longitudinal — following the same women over years.
A significant gap remains. Major studies excluded women with PCOS (up to 20% of the population), those with hysterectomies, and hormonal contraception users — leaving over a third of adult women unrepresented. Women in the Southeast and Southwest U.S. have also been largely absent from these cohorts. The research describing "normal" perimenopause may not reflect your experience.
The Biological Engine:
Compensated Failure
At the core of this transition is follicle depletion. As your egg supply decreases, your body doesn't quietly accept the shift — it compensates, and hard.
AMH (Anti-Müllerian Hormone) is produced by small follicles and reflects how many remain. As it declines, follicles appear to release from a biological "waiting room," activating earlier than normal. Inhibin B, produced by growing follicles, also drops — and as it does, it removes an important brake on FSH. FSH (Follicle-Stimulating Hormone) then rises, with your pituitary essentially turning up the volume to stimulate follicles that now require a stronger signal. This monotropic FSH rise is compensation in action.
Scientists use the STRAW framework (Stages of Reproductive Aging Workshop) to map where a woman is in this process:
Stage -2 (Early Transition): AMH and inhibin B are low, FSH is intermittently elevated — but from the outside, things may look relatively normal. Technically, elevated FSH is already causing follicles to grow faster and ovulate earlier, producing smaller follicles at ovulation than during peak reproductive years.
Stage -1 (Late Transition): The compensation breaks down. Periods can be absent for 60+ days, and the hormonal environment becomes more consistently low in estrogen and high in FSH.
Decoding the Cycle:
Why Your Period Is Acting Strange
Cycle irregularity during perimenopause follows identifiable patterns, even when it doesn't feel that way.
Researchers track Evidence of Luteal Activity (ELA) — whether ovulation actually occurred in a given cycle, measured by a meaningful rise in the progesterone metabolite pregnanediol glucuronide (Pdg). The findings are striking: in the early transition, about 81% of cycles show ovulatory evidence. In the year before the final period, only 23% do. That's not a gradual fade — it's a steep drop that mostly happens below the surface.
The LOOP Cycle
One of the most clinically significant findings from this research is a phenomenon called the Luteal-Out-of-Phase (LOOP) cycle. High FSH levels recruit a new wave of follicles during the previous cycle's luteal phase — before your period even arrives — triggering a second ovulation almost immediately after, or during, menstruation. The result is back-to-back progesterone surges and higher estrogen exposure in a compressed timeframe. LOOP cycles are one of the primary drivers of symptom volatility in perimenopause.
When ovulation doesn't happen at all, cycles diverge further. If estrogen rises but there's no LH surge, progesterone stays low and bleeding occurs when estrogen eventually falls. When estrogen doesn't rise at all, there's no menses — just a skipped period. Two women with "irregular cycles" may be experiencing very different hormonal realities.
Symptoms:
The Erratic Fluctuation Hypothesis
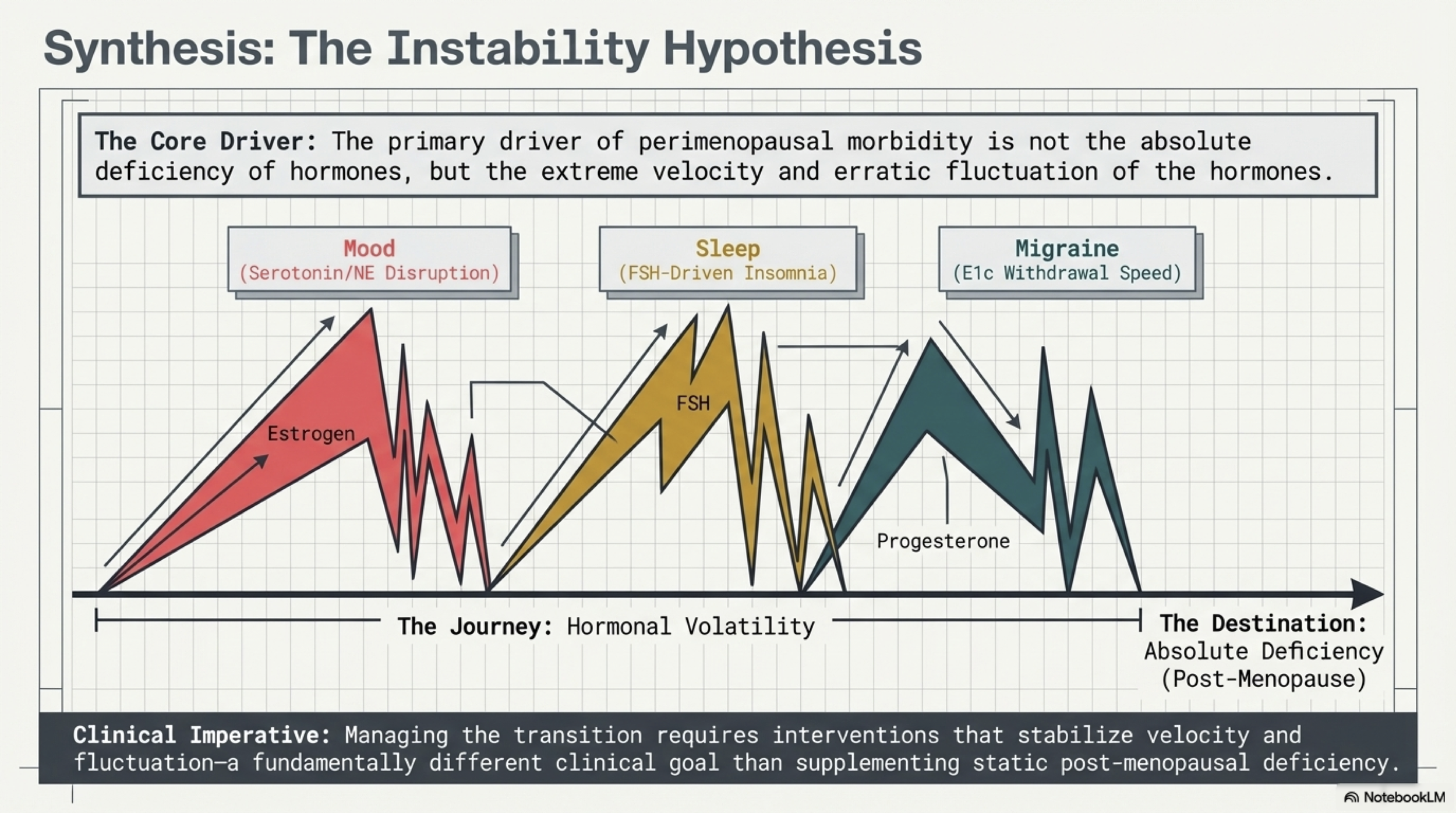
The dominant hypothesis in this field reframes perimenopausal symptoms entirely. Research suggests that the speed and amplitude of hormonal swings — the peaks and troughs — cause more disruption than absolute hormone levels alone. This is the Erratic Fluctuation Hypothesis, and it changes how we interpret nearly every symptom of this transition.
Mood
Women in the menopausal transition face a 1.5 to 3 times higher risk of depression compared to premenopausal women. Estradiol (E2) directly regulates the synthesis and metabolism of serotonin and norepinephrine. Wider fluctuations in both E2 and FSH are directly correlated with worse mood outcomes — the neurochemical mechanism is measurable.
Sleep
Sleep quality peaks during the periovulatory phase of the cycle. Difficulty falling or staying asleep is associated with lower estradiol and more rapidly increasing FSH — independently of vasomotor symptoms. Sleep disruption in perimenopause has its own hormonal mechanism, separate from hot flashes.
Headaches and Migraines
Researchers have identified a "migraine-specific hormone profile." Women who experience migraines show a measurably faster decline in the urinary estrogen metabolite E1c in the two days following the luteal peak — suggesting a fundamental difference in how quickly estrogen metabolizes, not just sensitivity to its presence.
Your Symptom Pattern Tends to Stay Consistent
Using Latent Class Analysis, researchers identified six distinct symptom profiles — from high-intensity across the board to largely asymptomatic. The key finding: most women remain in their symptom class throughout the entire transition. How you experience perimenopause early on is likely how you'll experience it throughout, which makes early awareness and early conversations with your provider more meaningful than most women are told.
Three Things Worth Knowing
Volatility is the story. The hormonal architecture of perimenopause is a compensatory system producing erratic peaks, and symptoms are largely driven by the speed of those changes.
A single lab test gives a limited picture. One FSH or estrogen reading is a snapshot of a moving target. Longitudinal tracking of AMH, FSH, and urinary metabolites like E1c tells a far more complete story. Feeling like something is shifting hormonally while labs "look normal" is entirely consistent with what the research shows.
Your hormonal fingerprint is individual. The research population used to define "normal" perimenopause excludes a significant portion of women. If your experience doesn't match the textbook description, that gap in the data may be part of why.
Source: Menstrual Cycle Hormone Changes Associated with Reproductive Aging and How They May Relate to Symptoms. Allshouse, A., Pavlovic, J., & Santoro, N. (2018). Obstetrics and gynecology clinics of North America, 45(4), 613–628.
Read the full review article here →https://doi.org/10.1016/j.ogc.2018.07.004